Integer Donec Amet Facilisis Aliquam Quis
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud.
Vel Etiam Viverra










Et Rhoncus Nunc, Faucibus
Internist Doctor

Internist Doctor

Internist Doctor

Nutrition Doctor

Pediatrician

Dermatologist

Pretium, Viverra Ultrices Habitant Posuere Sed Loremelo
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
Posuere pellentes
5000 available
Posuere pellentes
5000 available
Posuere pellentes
5000 available
Posuere pellentes
5000 available
Elit A Fringilla Lectus Id Ac Velit Ac. Dictum Pulvinar Dolor.
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
- Modern health laboratory
- Update information on the latest virus variants
- The best medicine for all patients
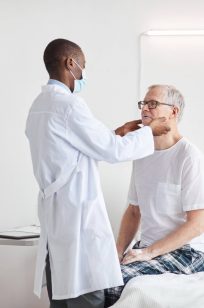
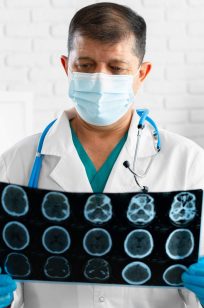


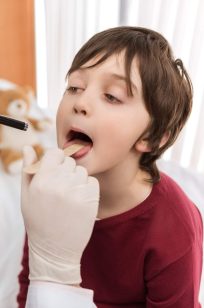
Elit a Fringilla Lectus Id Ac Velit Ac. Dictum Pulvinar Dolor.
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
- Cras sit sed nec a nunc
- Tempor mauris mauris in
- Nibh turpis praesent pretium
Integer At Mauris Augue Ultrices Eget Velit Scelerisque Risus Nisi. Sit Erat.
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec.


Doctor's Schedule Today


Subscribe Now
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec.






